Knee Osteoarthritis Injections: Your Complete Guide (2026)
Share this Post
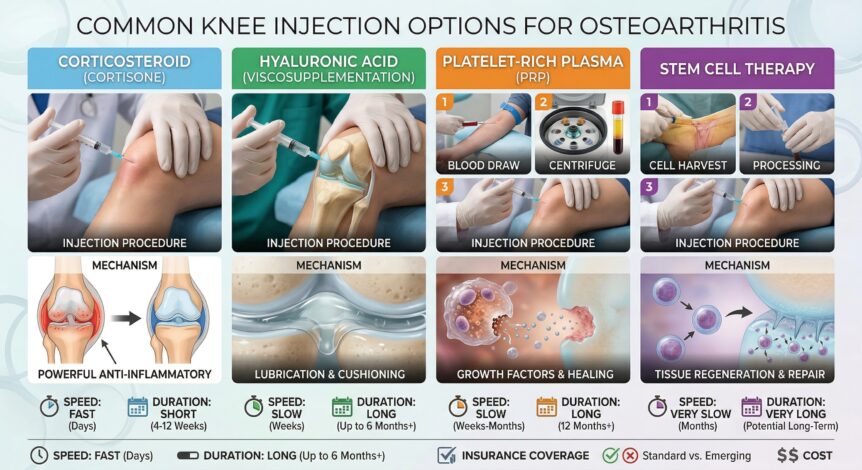
If your knees have been talking back to you lately, you’re far from alone. Knee osteoarthritis affects millions of adults, and one of the first questions patients ask is: “What can we do besides surgery?” The good news is that knee osteoarthritis injections have come a long way — from trusted options like hyaluronic acid to cutting-edge regenerative therapies. Here’s an honest, evidence-based look at where things stand today.
Hyaluronic Acid Injections: The Reliable Starting Point for Knee Osteoarthritis
You may know these as “gel shots” or viscosupplementation. Hyaluronic acid (HA) is a natural component of healthy joint fluid, and injecting it into an arthritic knee restores some of that lost cushioning and lubrication. It’s one of the most well-studied knee osteoarthritis injections available.
Current evidence shows HA injections work best for early-to-moderate arthritis. When they’re effective, patients typically experience meaningful improvements in pain and function lasting about six months. After that, benefits tend to fade — so a retreatment schedule of roughly every six months makes sense for good responders.
Who Benefits Most From Hyaluronic Acid?
HA injections are strongest as a bridge to delay surgery while you stay active, especially if anti-inflammatory medications aren’t an option or steroid injections haven’t provided lasting relief. They’re also a reasonable complement to exercise therapy, weight management, and bracing — not a standalone fix.
How Do Hyaluronic Acid Injections Compare to Steroid Injections?
This is one of the most common questions we hear. Steroid injections kick in faster but wear off sooner — and repeated use raises concerns about cartilage health over time. HA is slower to take effect but generally lasts longer, with a gentler metabolic profile. That makes HA particularly appealing for patients with diabetes, obesity, or those who want to avoid repeated steroid exposure.
PRP Injections: A Stronger Step Up for Knee Osteoarthritis
Platelet-rich plasma (PRP) therapy concentrates the healing growth factors from your own blood and delivers them directly into the joint. In the landscape of knee osteoarthritis injections, PRP has rapidly gained ground as a potent middle option between conventional treatments and experimental therapies.
Head-to-head research suggests PRP may outperform hyaluronic acid for both pain and function in many patients. Because PRP uses your own blood, the safety profile is strong. However, not all PRP is created equal — the way it’s prepared, the concentration of platelets, and the protocol all influence outcomes. This is an area where choosing an experienced provider matters significantly.
Regenerative Therapy for Knee Arthritis: The New Frontier
This is where things get exciting — and where setting realistic expectations becomes especially important. Several emerging regenerative approaches are generating real scientific interest for knee osteoarthritis.
Bone Marrow Concentrate (BMAC)
BMAC involves drawing a small amount of bone marrow (usually from the hip), concentrating its stem cells and growth factors, and injecting them into the knee. Among regenerative knee osteoarthritis injections, BMAC currently has some of the strongest clinical evidence — studies show it’s generally safe and associated with meaningful improvements in pain and function compared to controls.
Amniotic and Placental Tissue Products
These “off-the-shelf” products come from donated birth tissues and contain a rich mix of anti-inflammatory signals and growth factors. Early human studies show encouraging safety data and symptom improvements lasting up to 12 months in some patients.
Here’s the important caveat: these products likely work by calming inflammation and creating a better healing environment — not by literally regrowing cartilage. The actual stem cell content in many commercial products is quite low after processing. Studies so far are small, and we need larger, well-designed trials before making broad claims about efficacy.
Muse Cells: An Emerging Technology to Watch
Muse cells are a specialized subset of stem cells that show remarkable properties in laboratory research — they can home in on damaged tissue and differentiate into multiple cell types. Animal studies have demonstrated impressive cartilage repair results. However, as of 2026, Muse cell therapy for knee arthritis remains in early research stages with no large human trials yet. It’s a technology worth following, but not yet ready for mainstream clinical use.
Which Knee Osteoarthritis Injection Is Right for You?
There’s no single best injection for every patient. Instead, think of these options as a stepped approach based on where you are in your arthritis journey:
- Starting point: If you have early-to-moderate arthritis and want a well-established, low-risk option → hyaluronic acid is a solid first choice.
- Stepping up: If HA or steroids haven’t provided enough relief, or you want something potentially more effective → PRP is worth discussing with your provider.
- Going further: If you’re exploring regenerative options and understand they’re still evolving → BMAC has the most clinical support, while amniotic products and Muse cells are promising but more investigational.
Regardless of which path you choose, injections deliver the best outcomes as part of a comprehensive plan — not a standalone fix. The patients who see the greatest benefit are those who combine injection therapy with consistent exercise, attention to weight management, and an active partnership with their care team.
The Bottom Line on Knee Osteoarthritis Injections
We’re in a time when the options for managing knee arthritis without surgery are expanding rapidly. Some therapies are well-proven, others are still finding their footing — and that’s okay. The key is working with a provider who gives you the straight story about what the evidence supports, what’s still being studied, and what makes sense for your knee, your goals, and your life.
Have questions about which knee osteoarthritis injection might be right for you? Schedule a consultation — we’re here to help you sort through it honestly and without the hype.
Frequently Asked Questions About Knee Osteoarthritis Injections
When hyaluronic acid injections work for a patient, the benefits typically last about six months. After that, the effects tend to fade, so retreatment every six months is a common schedule for patients who respond well. Results vary — some patients notice improvement within a few weeks, while others take longer.
Research suggests PRP may produce stronger pain and function improvements than hyaluronic acid in many patients. However, HA remains widely used because of its strong safety record, accessibility, and regulatory clarity. The best choice depends on your specific situation, arthritis stage, and treatment goals — which is why a thorough evaluation matters.
Most stem cell and regenerative therapies for knee osteoarthritis are considered investigational and are not FDA-approved specifically for this use. Autologous options like bone marrow concentrate (BMAC) use your own cells and are performed under physician discretion. Amniotic and placental products face greater regulatory scrutiny. Always ask your provider about the regulatory status of any treatment.
For most patients with early-to-moderate knee osteoarthritis, hyaluronic acid injections are a well-established starting point. If those don’t provide adequate relief, PRP is a reasonable next step. Regenerative therapies like BMAC or amniotic products are typically considered when other conservative options have been insufficient and surgery isn’t desired.
