Gut Health and Chronic Pain: What Your Gut Has to Do With How You Feel
Share this Post
When you think about chronic pain, your stomach is probably not the first thing that comes to mind. But research is making one thing clear: gut health and chronic pain are deeply connected. The trillions of bacteria living inside your gut can drive inflammation, sensitize your nerves, and make pain worse — even in areas far from your abdomen. Understanding this connection opens a new door for treatment.
Your Gut Microbiome: More Than Just Digestion
Inside your gut live trillions of bacteria, viruses, and fungi. Together, this community is called the gut microbiome. These organisms do much more than break down food. They produce vitamins, regulate your immune system, and communicate directly with your brain through a highway called the gut-brain axis.
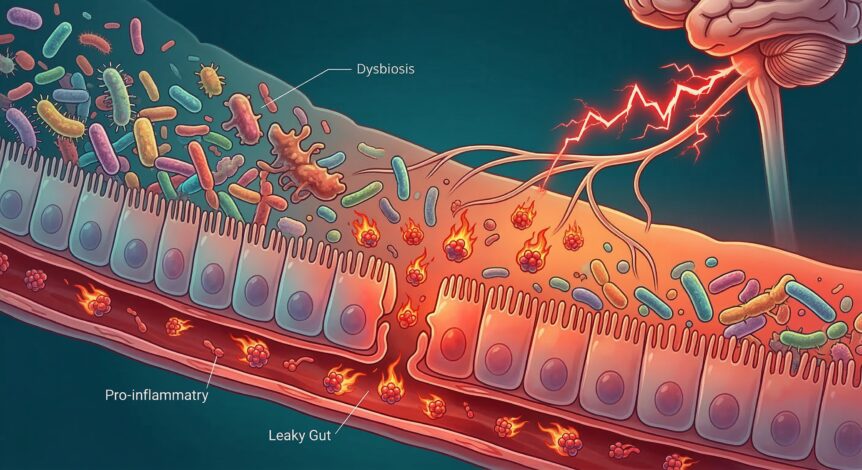
When your microbiome is balanced, these systems work quietly in the background. When it falls out of balance — a state called dysbiosis — problems start. A dysbiotic gut can trigger immune activation and send inflammatory signals throughout the body, including to your nervous system.
This is one reason why treating the gut has become an important strategy in non-surgical pain management.
What Is Leaky Gut and Why Does It Matter for Pain?
Think of your gut lining like a fine mesh screen. Under normal conditions, it allows digested nutrients to pass into your bloodstream while keeping bacteria and larger particles out. That screen is held together by proteins called tight junctions.
In leaky gut — the medical term is increased intestinal permeability — those tight junctions loosen. Bacteria, bacterial toxins, and partially digested food particles slip through into the bloodstream. Your immune system flags these as foreign invaders and mounts a response.
The result is low-grade, chronic inflammation. Over time, that inflammation sensitizes your nerve fibers. Signals that would normally feel like pressure or mild discomfort start to register as pain. This process is one mechanism behind widespread pain syndromes and central sensitization.
Research in people with fibromyalgia and chronic fatigue has found elevated markers of gut leakiness alongside higher levels of bacterial fragments in the bloodstream — and those with worse gut permeability tend to report worse symptoms.
The Gut-Brain-Pain Loop
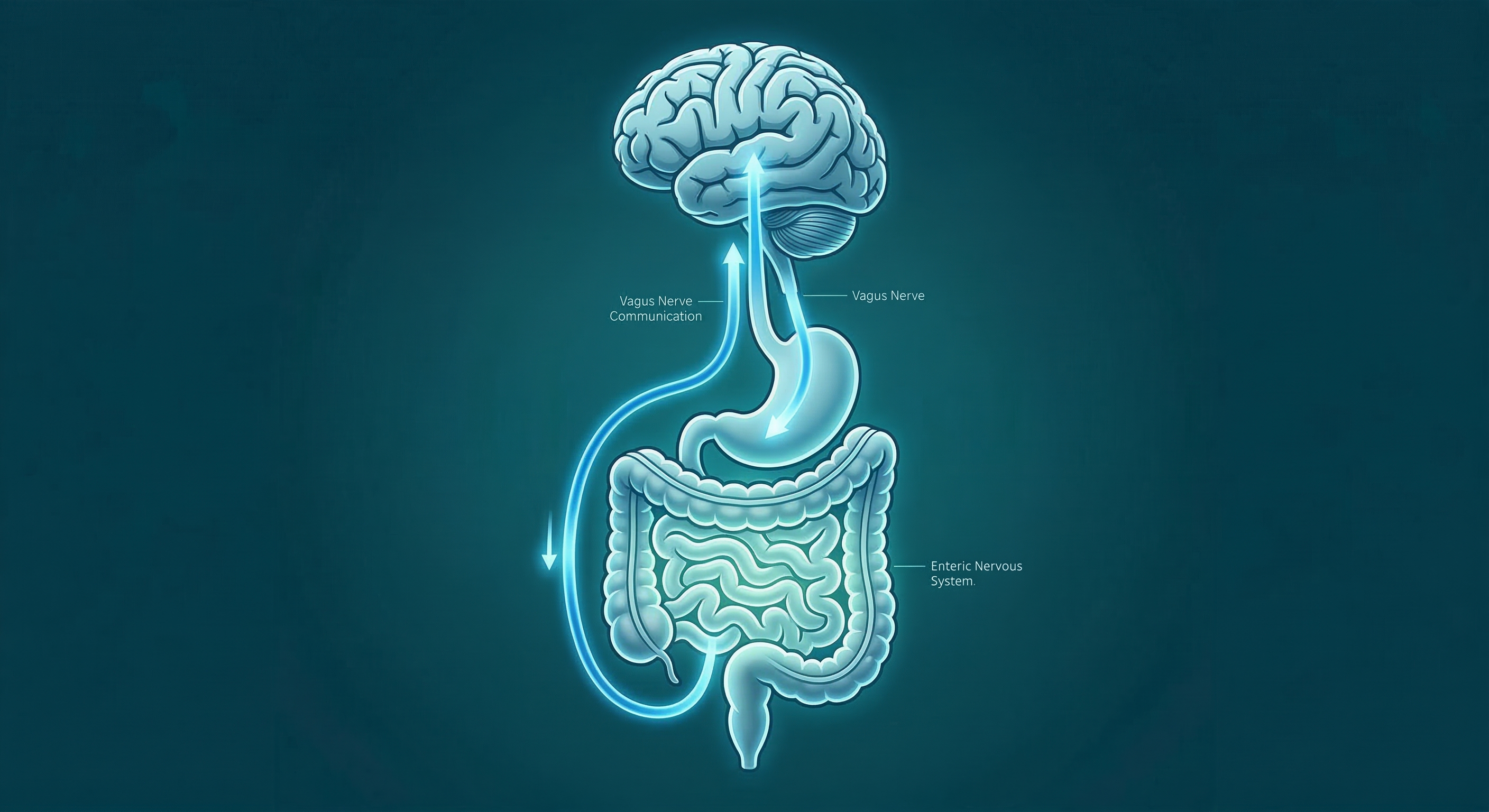
The vagus nerve serves as the primary communication highway between your gut and your brain — a key driver of chronic pain, inflammation, and nervous system sensitization.
Here is how the cycle works in plain terms:
- Gut bacteria fall out of balance (dysbiosis).
- The gut lining weakens and becomes more permeable.
- Bacterial toxins and food particles enter the bloodstream.
- The immune system activates and releases inflammatory signals.
- Those signals travel to the brain and spinal cord, sensitizing pain pathways.
- Ordinary sensations — movement, touch, temperature — start to feel painful.
Stress and poor sleep accelerate every step of this cycle. In turn, a disrupted gut worsens mood and sleep quality, which then amplifies pain. Breaking that loop requires addressing multiple entry points — including the gut.
Common pain presentations tied to this gut-brain disruption include:
- Chronic low back pain
- Fibromyalgia and widespread body aches
- Nerve pain and hypersensitivity
- Headaches
- Abdominal pain with bloating and gas
Can Probiotics Help With Chronic Pain?
Probiotics are live beneficial bacteria taken in supplement or food form. Common strains include Lactobacillus and Bifidobacterium species. They are designed to restore balance to a disrupted microbiome. Research on probiotics and pain is still developing, but early results are encouraging.
Fibromyalgia
In one clinical trial, adults with fibromyalgia took a combined prebiotic and probiotic supplement for 8 weeks. Participants reported lower pain scores, better sleep quality, and modest improvements in anxiety compared to those who took a placebo. The effect sizes were not dramatic, but they point to a real connection between gut bacteria and fibromyalgia symptoms.
Chronic Low Back Pain
A separate study focused on people with chronic low back pain and Modic type 1 changes — a specific pattern of inflammation visible on MRI. Participants took Lactobacillus rhamnosus GG for approximately 100 days. Pain scores improved modestly. Disability levels did not change significantly, but the direction of the results supports further investigation.
IBS and Abdominal Pain
Probiotics have the strongest evidence base in irritable bowel syndrome. Expert clinical guidelines recognize that probiotics, taken as a short trial of 4 to 12 weeks, can reduce abdominal pain and IBS symptoms in a meaningful proportion of patients. For people whose chronic pain overlaps with gut symptoms, this is worth addressing directly.
One important caveat: not all probiotics are equal. Different strains produce different effects. If a specific probiotic does not produce a noticeable benefit within 8 to 12 weeks, stopping and reassessing is the right call.
Diet: The Most Powerful Gut Lever You Have
If you want to improve gut health and reduce pain, diet is the most evidence-backed tool available. A Mediterranean-style, anti-inflammatory eating plan outperforms any single probiotic product in the current research.
This approach emphasizes:
- Vegetables and fruits in abundance
- Whole grains like oats, brown rice, and barley
- Beans, lentils, and legumes
- Nuts and seeds
- Olive oil as the primary fat source
- Fish and poultry over red meat
- Minimal sugar and processed foods
Studies in people with arthritis and fibromyalgia consistently show lower pain scores, better daily function, and improved energy and mood when patients adopt this style of eating. The effect is not instant, but it compounds over weeks and months.
Why Fiber Is Especially Important
Dietary fiber is the fuel your gut bacteria need to thrive. When beneficial bacteria ferment fiber, they produce short-chain fatty acids (SCFAs). These compounds help strengthen the gut lining, reduce inflammatory signaling, and send calming signals to the immune system and brain.
High-fiber foods include beans, lentils, oats, barley, fruits, vegetables, nuts, and seeds. Even a modest increase in fiber intake can shift the microbiome in a positive direction within a few weeks. Building a stronger gut lining over time is one of the most effective ways to address leaky gut and reduce the chronic inflammatory burden that amplifies pain.
Who Benefits Most From Gut-Focused Pain Care?
Gut-focused strategies are not limited to patients with obvious digestive complaints. The patients most likely to benefit include:
- People with fibromyalgia or widespread musculoskeletal pain
- People with chronic low back pain, especially with Modic changes on MRI
- People with chronic pain who also experience bloating, gas, irregular bowel habits, or abdominal discomfort
- People who notice that certain foods reliably worsen their pain or fatigue
- People who have had repeated courses of antibiotics or long-term use of acid-suppressing medications
For these patients, the gut is an underutilized lever — one that can improve pain, sleep, mood, and function when addressed thoughtfully alongside other treatments. [INTERNAL LINK: Regenerative Medicine / PRP page]
How We Address Gut Health at Core Medical & Wellness
At Core Medical & Wellness, we treat gut health as one piece of a larger pain picture. Diet and probiotics are add-on strategies, not replacements for established interventional and regenerative treatments. Our clinical approach follows a simple framework:
- Full history: We ask about pain patterns, sleep, mood, bowel habits, diet quality, antibiotic history, and medication use.
- Dietary foundation first: We recommend a Mediterranean-style, high-fiber eating plan as the starting point.
- Short probiotic trial when appropriate: For selected patients, we recommend an 8 to 12 week probiotic trial using one product at a time.
- Track and reassess: We monitor changes in pain, sleep, mood, and gut symptoms. If there is no clear benefit, we stop the probiotic rather than continuing indefinitely.
The goal is straightforward: calm systemic inflammation, support a healthier gut lining, and reduce the constant noise driving your nervous system to stay on high alert.
A Note on Safety
Probiotics are considered safe for most healthy adults. They require more caution in people with severely weakened immune systems, serious heart valve conditions, or complex gastrointestinal histories. Always discuss any new supplement with your physician before starting, particularly if you are managing multiple health conditions or taking multiple medications.
Frequently Asked Questions
What is leaky gut and how does it cause chronic pain?
Leaky gut occurs when the gut lining becomes too permeable, allowing bacteria and toxins into the bloodstream. Your immune system responds with chronic inflammation, which over time sensitizes nerves and amplifies pain signals throughout the body — even in areas far from the gut.
Can probiotics help reduce chronic pain?
Early clinical research shows probiotics can modestly reduce pain in fibromyalgia, chronic low back pain, and IBS. They are most effective as add-on support alongside other treatments. Strain selection and trial duration matter — benefits vary significantly by individual and by product.
What foods help with gut health and pain?
A Mediterranean-style, high-fiber diet is the strongest evidence-based dietary strategy for both gut health and pain reduction. Focus on vegetables, fruits, whole grains, legumes, olive oil, and fish. Reduce sugar, ultra-processed foods, and excess red meat.
Who benefits most from gut-focused pain treatment?
People with fibromyalgia, widespread body pain, chronic low back pain with Modic changes, or chronic pain combined with IBS-type digestive symptoms are the best candidates for gut-focused care strategies.
The Bottom Line
Your gut does not exist in isolation from your pain. The bacteria in your microbiome, the integrity of your gut lining, and the foods you eat all influence how inflamed your body is and how sensitive your nervous system becomes. Addressing gut health will not replace interventional pain treatment, but it can meaningfully improve how you feel and how well other treatments work.
If you have chronic pain and want to explore whether leaky gut or gut dysbiosis is part of your story, our team at Core Medical & Wellness can help you build a practical, evidence-informed plan. Contact us today to schedule a consultation at one of our New Jersey locations.
