Wolverine Stack for Pain: BPC-157 + TB-500 Recovery & Chronic Pain Guide (2026)
Share this Post
Medical Disclaimer: This article is for learning purposes only. It is not medical advice. BPC‑157, TB‑500, and the Wolverine stack are not approved by the FDA for any medical use. Always talk with your doctor before trying any peptide therapy. If you have a medical emergency, call 911.
The Wolverine stack is one of the most talked-about peptide combos in health and wellness right now. It pairs two peptides — BPC‑157 and TB‑500 — with the goal of helping your body heal faster. People originally used it for sports injuries and post-surgery recovery. But now, more people are asking whether it could also help with chronic pain — the kind that sticks around for months or years.
In this guide, we explain what these peptides are, what the science says so far, the risks you should know about, and what changed with the FDA in 2026.
What Is the Wolverine Stack?
The Wolverine stack is a nickname for taking BPC‑157 and TB‑500 together. It is named after the comic book character who heals super fast. People use this combo hoping it will speed up recovery from muscle tears, tendon injuries, sprains, and surgery. Some doctors are also looking at whether it might help with long-lasting pain from things like bad knees, joint problems, and inflammatory conditions.
Both peptides are usually given as small shots under the skin. Some people take BPC‑157 by mouth for stomach issues, but we do not have good data on how well that works.
What Is BPC‑157?
BPC‑157 stands for “Body Protection Compound‑157.” It is a small protein made in a lab, based on a natural protein found in your stomach. In animal studies, it seems to help tendons and ligaments heal faster, grow new blood vessels in hurt areas, calm down inflammation, and protect the stomach lining.
These results are interesting, but almost all of them come from studies on rats and mice — not people.
What Is TB‑500?
TB‑500 is a lab-made version of part of a natural protein called thymosin beta‑4. This protein helps your body repair damaged tissue. In animal research, it helps healing cells move to injured areas faster, supports new blood vessel growth, and reduces scar tissue.
TB‑500 is thought to work throughout your whole body, not just in one spot. Some early research also suggests it might help protect nerves, which could matter for certain types of chronic pain.
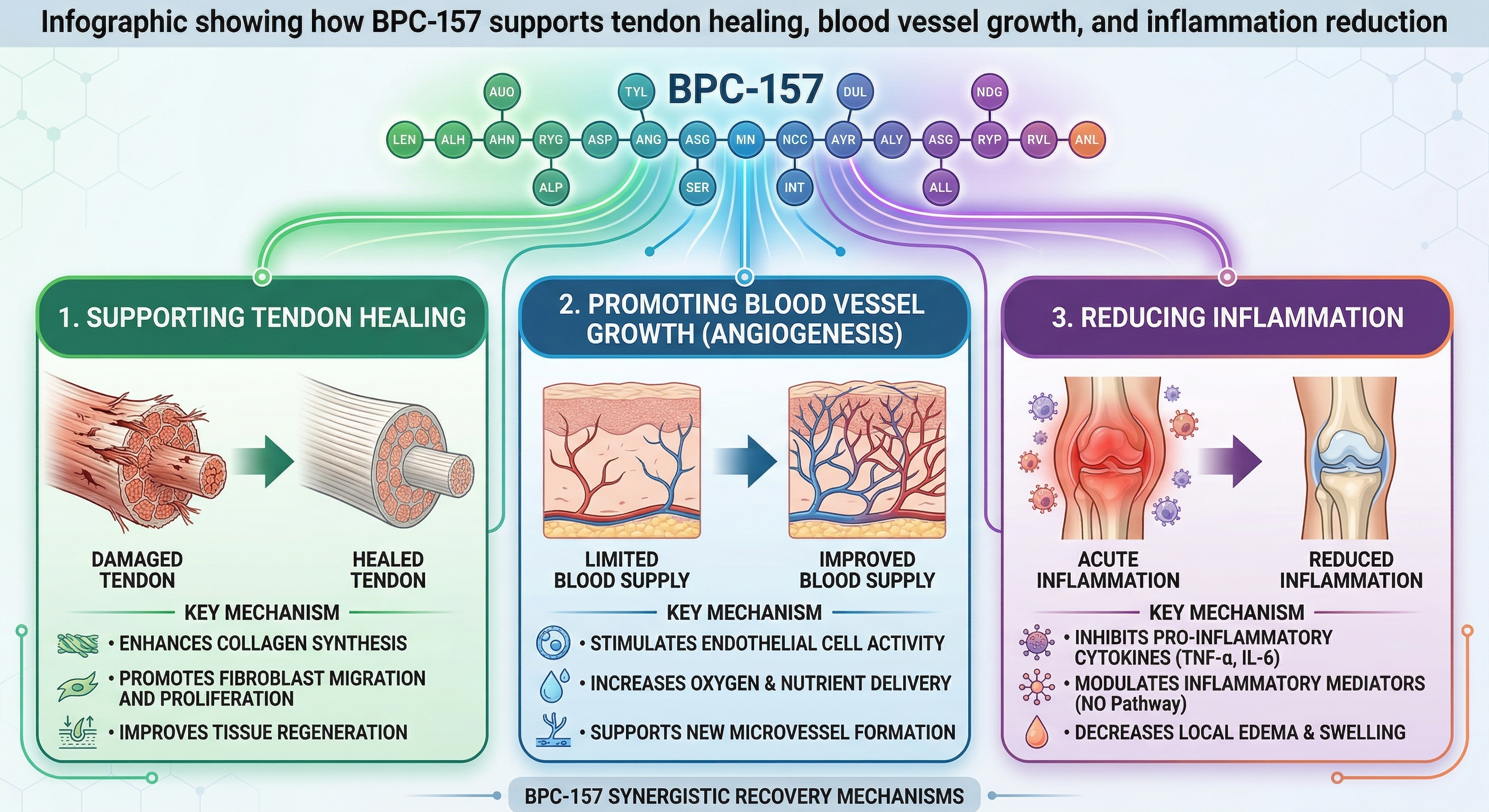
BPC-157 supports recovery through three key mechanisms identified in preclinical research: enhancing tendon and ligament healing via collagen synthesis, promoting new blood vessel growth (angiogenesis) to improve oxygen delivery, and reducing inflammation by inhibiting pro-inflammatory cytokines like TNF-α and IL-6. These findings are based on animal studies and have not been confirmed in large human trials.
Why Do People Combine Them?
The idea is simple. BPC‑157 works more at the local level — right where you are hurt. TB‑500 works more throughout your entire body. Fans of the Wolverine stack believe that using both together covers more ground than either one alone.
This makes sense on paper, but there are no large human studies proving the combo works better than using just one.
The Wolverine Stack for Surgery Recovery
The most common reason people try the Wolverine stack is to bounce back faster after surgery or a bad injury. In animal studies, BPC‑157 helped repaired tendons get stronger, and TB‑500 reduced the scar tissue that can limit your movement after an operation.
For patients recovering from procedures like rotator cuff repair, ACL reconstruction, or joint replacement, the idea of speeding up healing is very appealing. However, no large human trials have tested the Wolverine stack for post-surgical recovery. The positive stories you hear are personal reports, not scientific proof.
The Wolverine Stack for Chronic Pain
This is where things get especially interesting. Chronic pain is different from the sharp pain you feel right after an injury. Chronic pain lingers for months or years, often because of ongoing inflammation, nerve changes, or tissue that never fully healed. Millions of Americans deal with it every day.
While the research is still very early, a few small human studies hint that BPC‑157 might help with certain chronic pain conditions.
Chronic Knee Pain
In one small study, 16 patients with ongoing knee pain got BPC‑157 injections in their knee joint. When researchers checked back 6 to 12 months later, 14 out of 16 — about 87% — said their pain was much better. The study was small and had no comparison group, but the fact that relief lasted many months is noteworthy.
Chronic Bladder Pain
A 2024 pilot study looked at 12 women with a painful bladder condition called interstitial cystitis. All 12 had already tried the only FDA-approved drug for it and it did not work. After one BPC‑157 injection into the bladder, 10 out of 12 patients said their symptoms went away completely. The other 2 said about 80% of their symptoms improved. No side effects were reported, and some patients felt better within just 2 weeks.
Why This Matters
Traditional painkillers like opioids work by blocking pain signals. BPC‑157 and TB‑500 take a different approach — they try to actually repair the damaged tissue and reduce the inflammation that causes the pain in the first place. If this approach holds up in bigger studies, it could be a meaningful option for people whose chronic pain has not responded to standard treatments.
That said, these studies are tiny. Fewer than 30 total patients have been studied across all published BPC‑157 human trials. We need much bigger, better-designed studies before we can call this a proven treatment.
What Does the Research Actually Show?
Here is an honest look at where the science stands as of early 2026:
- Animal studies are promising. Decades of research show consistent healing benefits in rats and mice.
- Human studies are very limited. Only three small BPC‑157 studies in people have been published. None had a placebo control group.
- TB‑500 has zero published human trials.
- No one has studied the full Wolverine stack combo in people.
- Neither peptide is FDA-approved for anything.
Other things — like physical therapy, good sleep, better nutrition, and time — can also explain why people feel better. The placebo effect is also very real, especially with pain.
Common Dosing Patterns (Not Recommendations)
These details are not medical advice. They simply describe what people commonly report online and in some clinics.
BPC‑157: Usually given as a small shot under the skin near the sore area. Common doses are 200 to 500 micrograms once or twice a day, for 2 to 6 weeks. For chronic conditions, some people use longer cycles.
TB‑500: Usually given as a shot under the skin or into the muscle. Common doses are 2 to 5 milligrams per week, split into 2 or 3 shots, for 4 to 8 weeks.
These are experimental patterns. No standard medical guidelines exist.
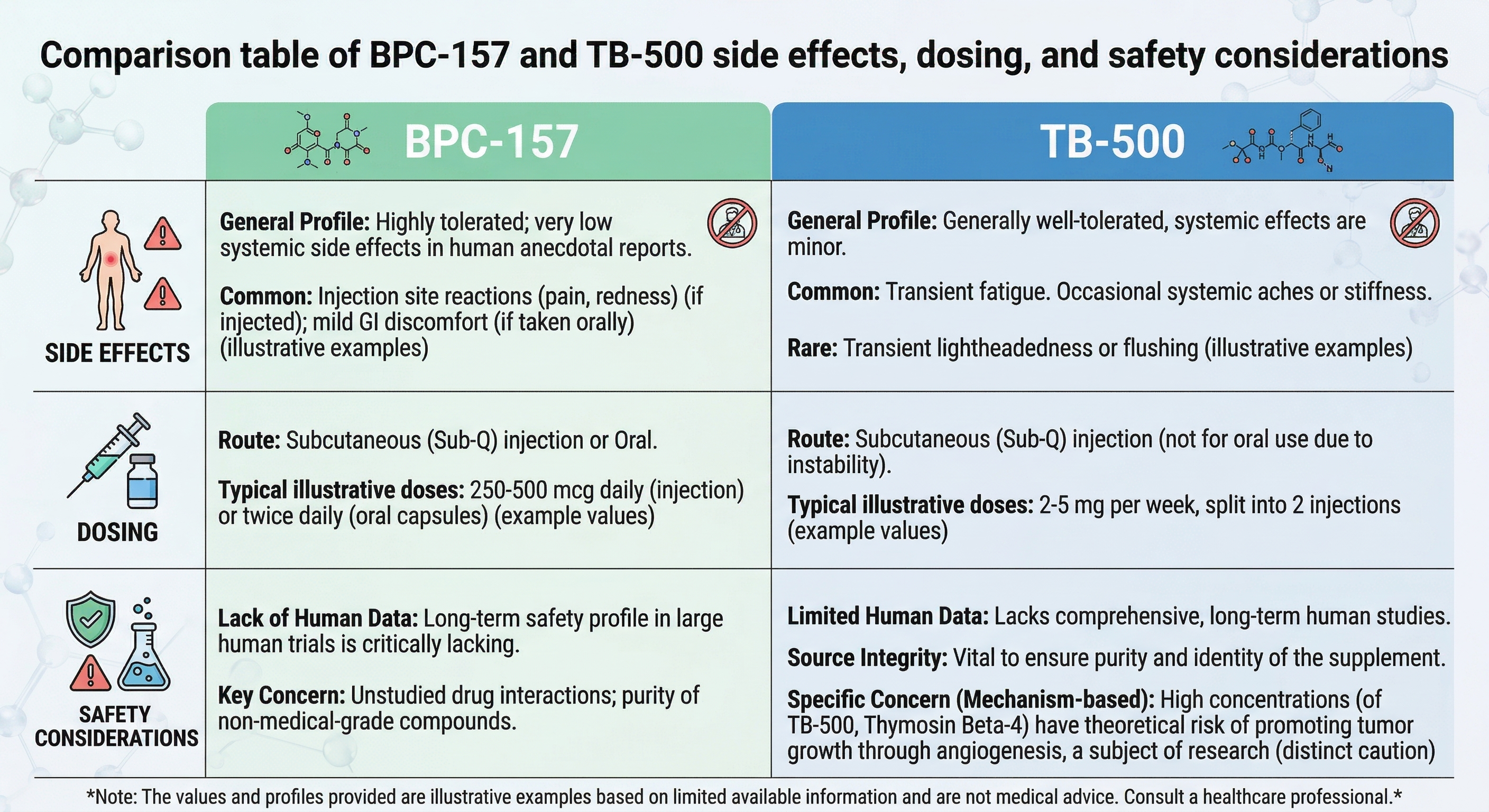
Side-by-side comparison of BPC-157 and TB-500 across three categories: reported side effects, illustrative dosing patterns, and safety considerations. Both peptides lack long-term human safety data, and the values shown are illustrative examples — not medical recommendations. Always consult a healthcare professional.
Safety: What Are the Risks?
Because there are so few human studies, we do not have a clear picture of long-term safety. This is especially important for chronic pain patients who might use these peptides for a longer time.
Side Effects People Report
The most common complaints are mild: pain, redness, or bruising where the shot is given. Some people also mention nausea, headaches, dizziness, tiredness, or sleep changes. It is hard to know how often these are truly caused by the peptides.
Bigger Concerns
Doctors have raised some serious “what if” questions. These peptides help cells grow and build new blood vessels. In theory, that could also feed hidden cancers — though this has not been shown in people. They may also change how the immune system works, which could be a problem if you have an autoimmune condition. And products from unregulated online sellers can be contaminated or have the wrong dose.
If you have a history of cancer, autoimmune disease, or are pregnant or breastfeeding, most doctors say to stay away.
Are These Peptides Legal? The 2026 FDA Update
What Happened Before
In 2023 and 2024, the FDA told pharmacies to stop making BPC‑157 and TB‑500 because there was not enough safety data. Many patients who wanted them had to turn to sketchy “research chemical” websites.
What Changed in 2026
In early 2026, the government announced plans to let about 14 peptides — including BPC‑157 and TB‑500 — be made again by licensed pharmacies with a doctor’s prescription. This is good news for quality and safety, but it does not mean the FDA has approved these peptides as safe and effective. As of March 2026, availability may still vary by state.
What This Means for You
You may soon be able to get these peptides from a real pharmacy instead of a random website. That is a much safer option. But they are still experimental, insurance probably will not cover them, and you should make this decision with your doctor — not on your own.
What About Sports?
If you compete in any sport, this is critical. BPC‑157 and TB‑500 are banned by WADA (the World Anti-Doping Agency) and by the NFL, UFC, NCAA, and other organizations. Using them can mean failed drug tests, suspensions, and lost titles. Always check with your sport’s rules first.
Should You Try the Wolverine Stack?
- It is promising but unproven. Animal data look good. Human data are extremely limited.
- Chronic pain applications are very early. The small studies on knee pain and bladder pain are interesting, but they involved fewer than 30 patients total.
- The basics still matter most. Physical therapy, sleep, nutrition, stress management, and good rehab are the foundation of recovery and pain management.
- Peptides are not a shortcut. If you use them, they should be one small part of a bigger plan — not a replacement for proven treatments.
- Where you get them matters. Use a licensed pharmacy with a real prescription, never an unregulated website.
- Talk to your doctor first. That is the safest and smartest next step.
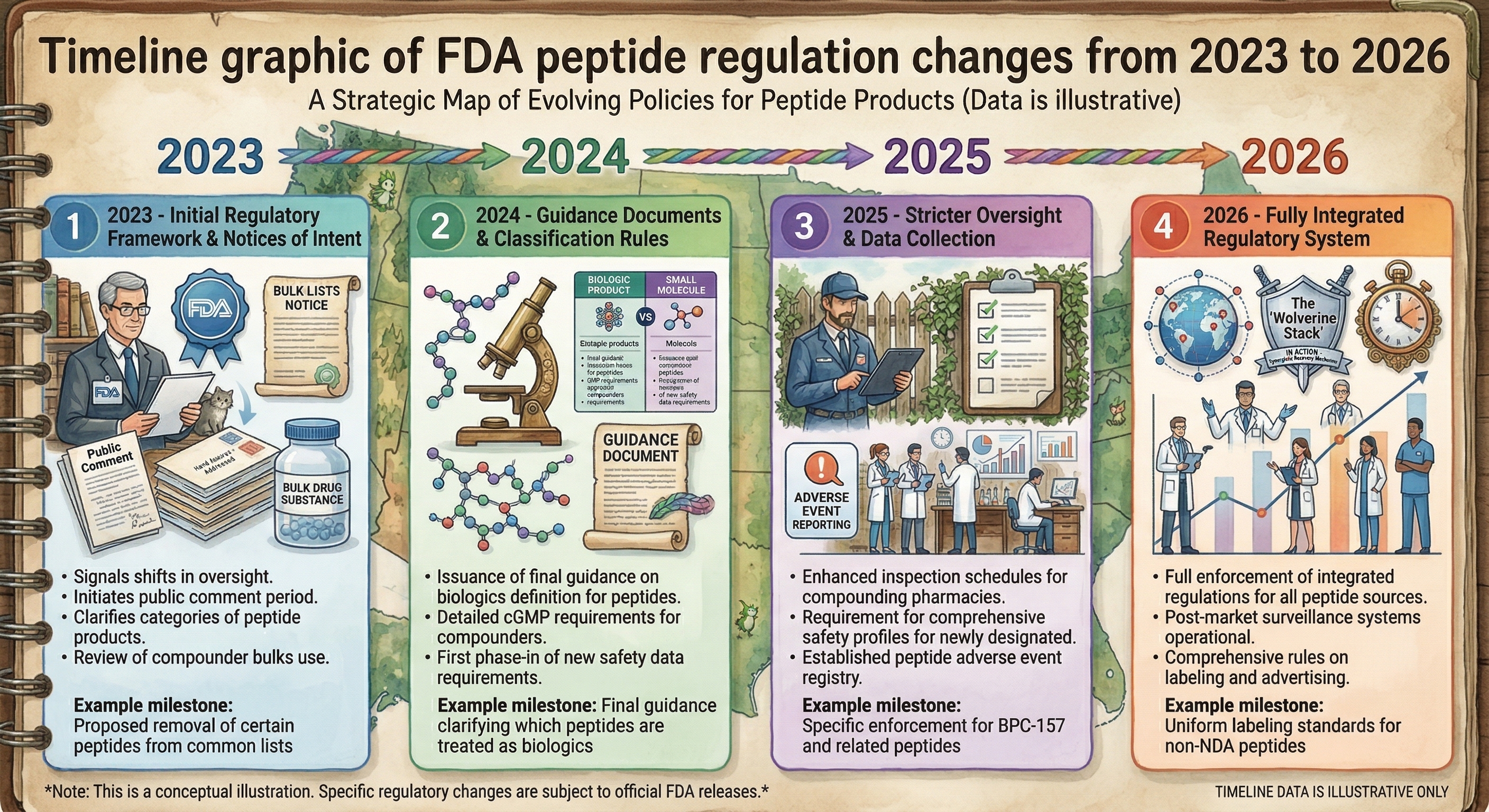
How FDA peptide regulation has evolved from 2023 to 2026 — from initial bulk drug substance reviews and compounding pharmacy restrictions to the 2026 framework that allows licensed pharmacies to compound peptides like BPC-157 and TB-500 again under a doctor’s prescription. This is a conceptual illustration; specific regulatory details are subject to official FDA releases.
Frequently Asked Questions
What is the Wolverine stack used for?
It combines BPC‑157 and TB‑500 to try to speed up healing from injuries and surgery. Some people also use it for chronic pain in joints, tendons, and inflammatory conditions. It is not FDA-approved.
Can the Wolverine stack help with chronic pain?
Early data are limited but interesting. In small studies, most patients with chronic knee pain or chronic bladder pain reported major improvement after BPC‑157 treatment. But these studies were tiny and had no placebo group. Much more research is needed.
Is the Wolverine stack FDA-approved?
No. As of 2026, the FDA allows licensed pharmacies to make these peptides with a prescription, but that is not the same as approving them as safe or effective.
What are the side effects?
Common reports include soreness at the injection site, nausea, headache, and tiredness. Long-term risks are unknown. Theoretical concerns include effects on cancer growth and immune function.
Is it legal in 2026?
It is becoming easier to get legally. Federal officials are letting licensed pharmacies compound these peptides again with a prescription. Rules are still being finalized and may vary by state.
Can athletes use it?
No. Both peptides are banned by WADA and major sports leagues. Using them can lead to failed tests and suspensions.
How is this different from opioids?
Opioids block pain signals. BPC‑157 and TB‑500 aim to repair damaged tissue and reduce inflammation at the source. This approach is appealing, but it has not been proven in large human trials.
How long is a typical cycle?
BPC‑157 is usually used for 2 to 6 weeks. TB‑500 for 4 to 8 weeks. Some people with chronic conditions use longer cycles. No official medical protocol exists.
